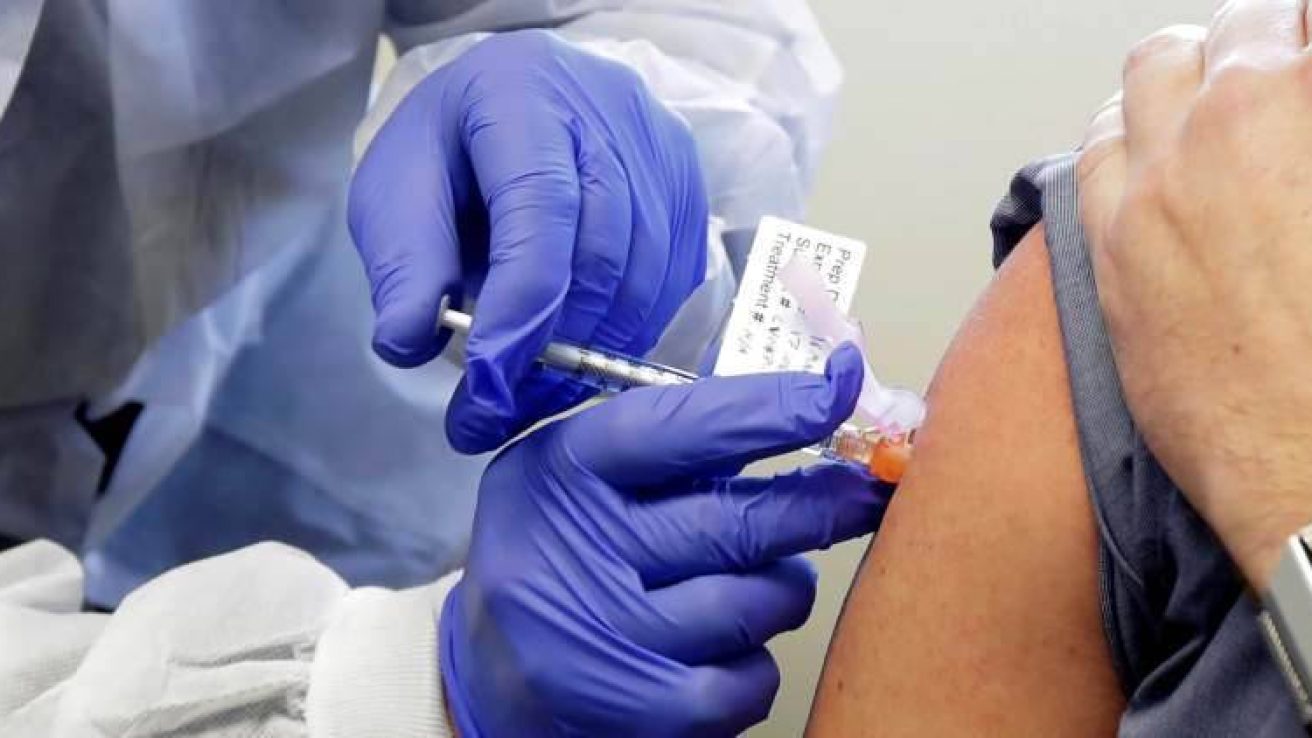
In this MD Newsline exclusive interview with obstetrician and gynecologist Dr. Wendy Goodall McDonald, we discuss the perception of vaccination in general and the perception of the COVID-19 vaccine in particular among minority patients.
MD Newsline:
Can you speak to the question, will minority patients get vaccinated for COVID-19?
Dr. Wendy McDonald:
“During COVID-19, we’ve seen significant health disparities when it comes to the impact of the virus on ethnic populations. African American patients are significantly more likely to have severe illness and die than white Americans, as are Latino Americans. They are also significantly more likely to have higher mortality.
As we approach [the topic of] vaccination for COVID-19, we have to remember that there’s a lot of medical distrust historically in this country with relation to experimentation and use of certain new and nuanced medications on populations that may be underrepresented or oppressed. And so, I don’t expect a large proportion of those in the ethnic populations to be first in line to get a vaccine for COVID even though we are more affected when it comes to the severity of disease.
However, I think it’s always important to present what’s available to all of your patients. Do not expect that a person will not want it because they’re of an ethnic background. Do not offer the vaccination less because the person is of an ethnic background. But know that there may be some pushback. There may be some hesitancy, and it is founded on history.
So, just as I have said with my flu vaccinations, I offer the flu vaccine to everybody of all ethnic backgrounds. And if a person does not want the flu vaccine, I ask them, ‘what is your concern? Why don’t you want it?’ And I often will say, ‘I’m just curious,’ because I don’t want them to think that this is an antagonistic relationship that they’re going to have to argue their point. I just want to know where their thoughts are.
And depending on what they say, I may be able to offer them some comfort, or I may even be able to present to them reasons why they should consider it. For example, with the flu vaccine in my pregnant patients, I’ll tell them, ‘you should get the flu vaccine for these reasons: one, it will help to protect you during the flu season when you are most susceptible as a pregnant person, [two,] it will protect your baby who will be born during flu season, and [three,] there’s a pandemic [going on] with COVID-19.
So often, with that information, a person will either decide, ‘maybe I do want it,’ or if they refuse it, [at least] they’ll know why they’re refusing it. When the COVID-19 vaccine is available [to everyone], and we have data for its safety, I plan to offer it to all of my patients. I expect that a good proportion will not want it, but some will. And those who take it, great. But those who don’t, I will make sure that they understand the risks, benefits, and alternatives of their decision, and I will do it in a way that’s not antagonistic.
I’ll also often tell my patients, ‘if you don’t want it, I won’t disown you. I will still be your doctor.’ So that they know that they will still have their care with me, they will still feel comfortable with me, that we can have these conversations without fear of repercussion.”
Responses have been condensed and lightly edited.