Biparametric prostate MRI reduces biopsy rates more than PSA screening alone and detects clinically relevant prostate cancers that PSA screening misses.
The prostate-specific antigen (PSA) blood test is still used for prostate cancer screening after randomized clinical trials showed a reduction in prostate cancer mortality rates. Several serological and imaging techniques have been explored to enhance its diagnostic accuracy. As an additional test to PSA, prostate multiparametric MRI (mpMRI) has been studied to better identify patients who need a prostate biopsy for the presence of aggressive types of prostate cancer. Randomized clinical trials have demonstrated that mpMRI is superior to PSA alone in predicting the presence of clinically relevant prostate cancer.
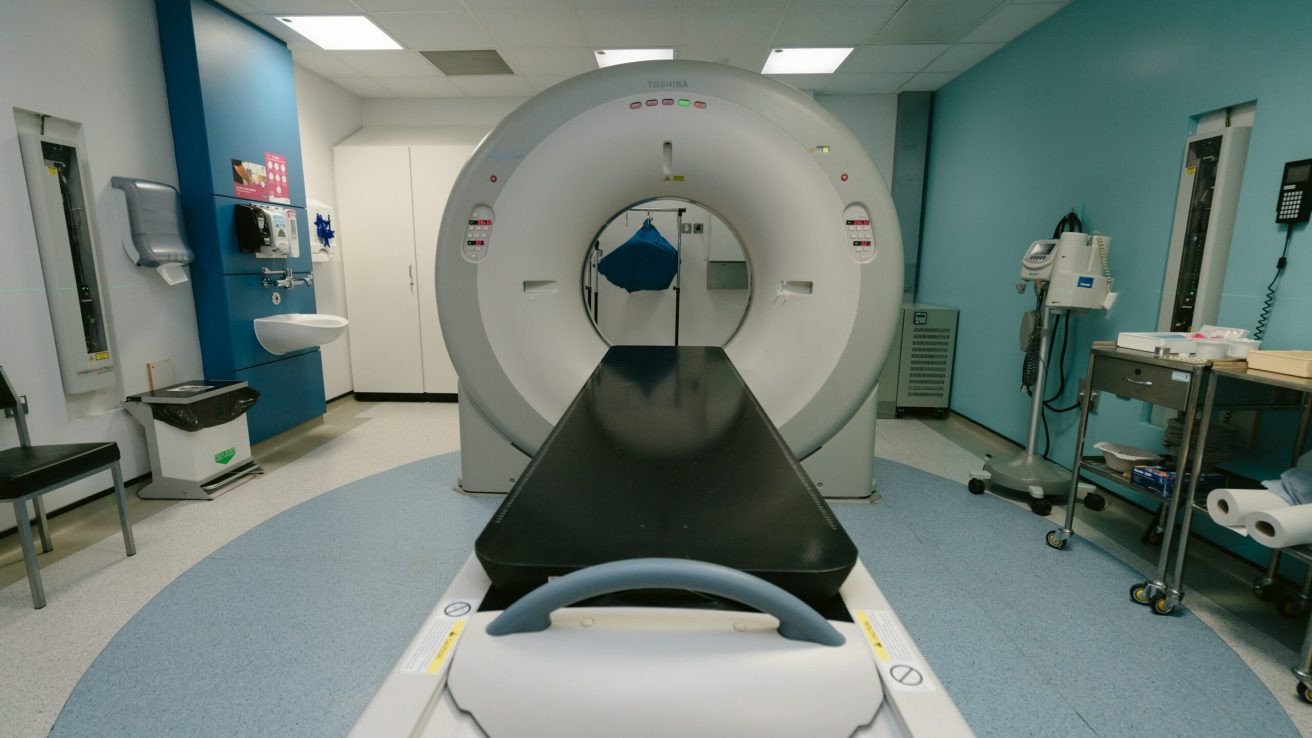
This Phase III randomized controlled trial, published in BMJ Open, aimed to compare the prostate cancer detection rates of patients screened for prostate cancer using serum prostate-specific antigen (PSA) against magnetic resonance imaging (MRI).
Participants were asymptomatic men aged 50 or older with no history of PSA screening within the previous three years, a negative digital rectal exam, and no prior prostate biopsy. Intervention patients were advised to obtain a prostate biopsy if their PSA level was ≥ 2.6 ng/mL (PSA arm) or their PIRADS score was four or five (MRI arm). Participants in the MRI arm with higher PIRADS scores were more likely to have had an end-of-study PSA. Adenocarcinoma on prostate biopsy, prostate biopsy rates, and clinically relevant prostate cancer occurrence were also compared.
Randomization was performed on 525 patients, with 266 assigned to the PSA arm and 248 to the MRI arm. In the PSA arm, 48 individuals had abnormal PSA levels, and 28 (58%) consented to a prostate biopsy. Twenty-five patients in the MRI arm with a PIRADS score of four or five consented to a biopsy.
It was found that, compared to PSA, the relative risk for MRI to indicate the need for a prostate biopsy was 0.52. The cancer detection rate for patients in the PSA arm was 29% compared to 63% in the MRI arm (p=0.019), with a larger proportion of clinically serious cancer diagnosed in the MRI arm (73% vs. 50%). The relative risk for cancer detection and clinical significance was 1.89 with MRI, compared to 2.77 with PSA.
It was concluded that, as a standalone screening test, prostate MRI decreased the rate of prostate biopsies. The MRI arm revealed a greater number of clinically relevant tumors, although this difference did not achieve statistical significance. More patients were willing to undergo prostate biopsies when advice was based on MRI data.
Reference:
Nam, R., Patel, C., Milot, L., Hird, A., Wallis, C., Macinnis, P., Singh, M., Emmenegger, U., Sherman, C., & Haider, M. A. (2022). Prostate MRI versus PSA screening for prostate cancer detection (the MVP Study): a randomised clinical trial. BMJ Open, 12(11), e059482. https://doi.org/10.1136/bmjopen-2021-059482