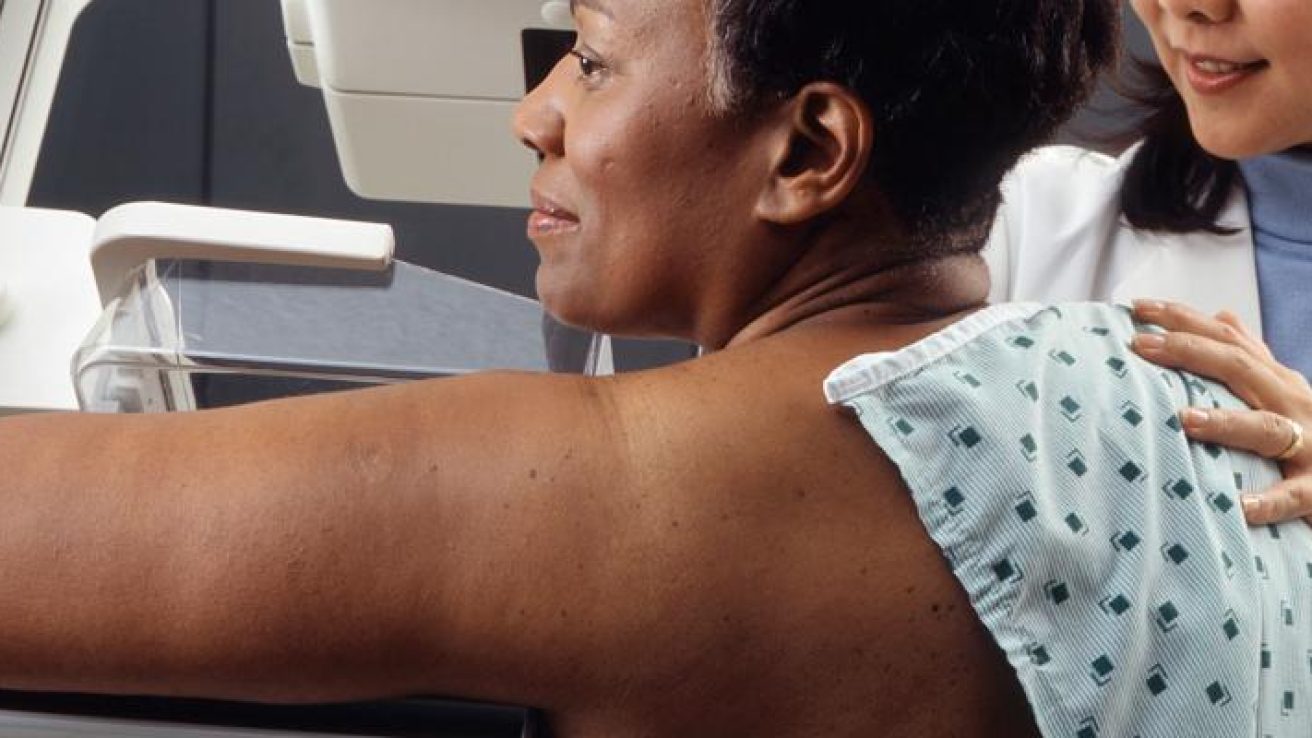
A recent study led by Dr. Emily Ambinder at Johns Hopkins University analyzed how race in America affects breast cancer screening with digital breast tomosynthesis (DBT). Dr. Ambinder was interested in DBT for breast cancer screening, specifically, because DBT is superior to 2D full-field digital mammography (FFDM) in detecting breast cancer and requires less repeat imaging for suspicious findings. Of note, DBT has been fully covered by Medicare and Medicaid since 2015.
The study participants included 140,346 female adults screened at Johns Hopkins University and affiliated sites from 2013 to 2020. Of these participants, 97,023 received DBT and 43,323 received FFDM. The study demographics included middle-aged and elderly white, Black and Asian American women. Statistical analysis was adjusted for year and race.
The study ultimately found that Black women and Asian American women were significantly less likely (p < 0.001) to have a screening study with DBT compared to white women (Black women: OR: 0.51; 95% CI: 0.48 to 0.70; Asian American women: OR: 0.59; 95% CI: 0.57 – 0.80).
The study also supported DBT’s superiority to FFDM in detecting breast cancer in white women (p < 0.0001), Black women (p = 0.001) and Asian American women (p = 0.01). However, in Asian American women, DBT was not superior to FFDM in requiring less repeat imaging for suspicious findings (p = 0.97), like it was in white women (p < 0.001) and Black women (p = 0.001).
The study concludes that racial disparities in breast cancer screening persist despite advances in screening. A call to action is made advocating for further research on how race, socioeconomic status, insurance status and educational attainment impact equitable access to DBT and breast cancer survival outcomes [1].
Source:
[1] Racial disparities persist despite with uptake of digital breast tomosynthesis (DBT) for breast cancer screening. (2020). https://cancerres.aacrjournals.org/content/81/4_Supplement/SS1-02