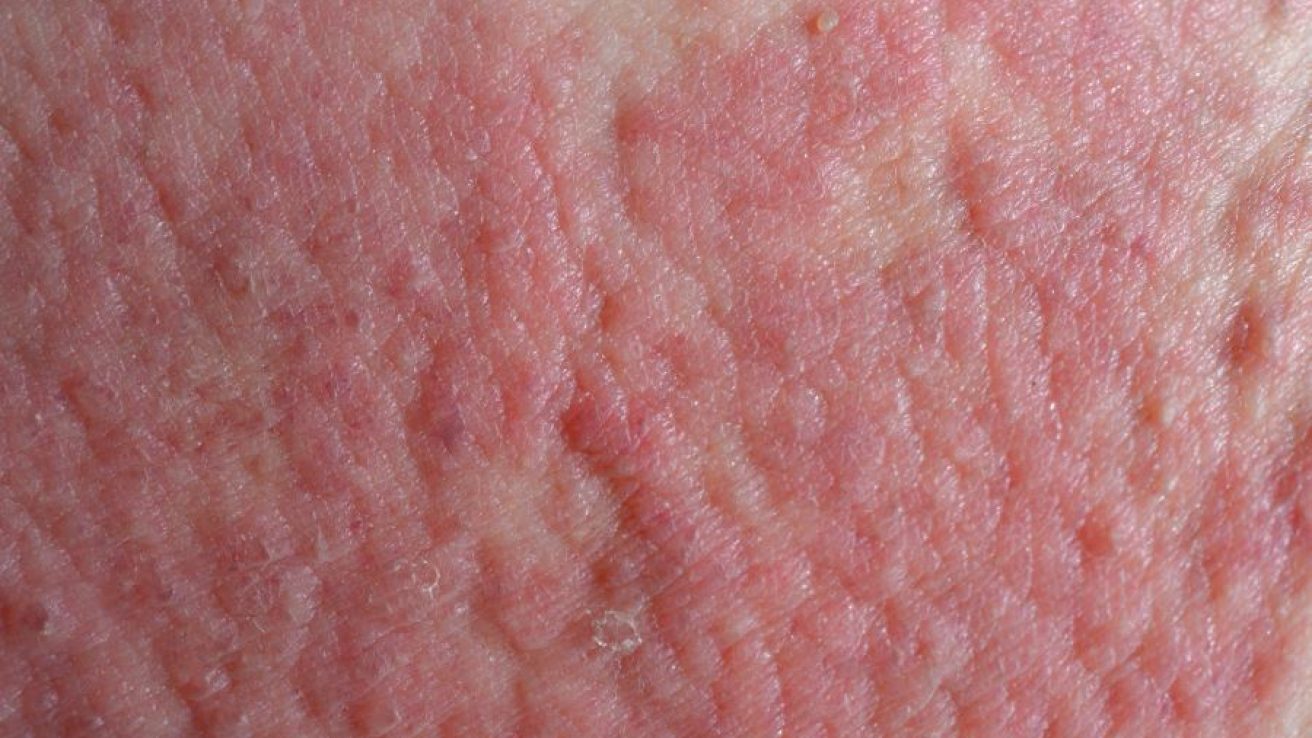
WEDNESDAY, Feb. 3, 2021 (HealthDay News) — There is an increased risk for all-cause and cause-specific mortality among patients with atopic eczema, particularly among those with the most severe or predominantly active disease, according to a study published online Jan. 27 in the Journal of Allergy and Clinical Immunology.
Richard J. Silverwood, Ph.D., from the London School of Hygiene and Tropical Medicine, and colleagues assessed whether adults with atopic eczema were at increased risk for death overall and whether the risk varied by atopic eczema severity and activity. The analysis included 526,736 patients identified through U.K. primary care electronic health care records, as well as 2,567,872 matched controls with a median follow-up of 4.5 years.
The researchers found limited evidence of an increased hazard for all-cause mortality in those with atopic eczema (hazard ratio, 1.04), owing to the low mortality rates overall, but there were somewhat stronger associations (hazard ratios, from 1.08 to 1.14) for deaths due to infectious, digestive, and genitourinary causes. There was a markedly increased mortality risk associated with eczema severity and activity. Patients with severe atopic eczema had a significantly increased risk for mortality (hazard ratio, 1.62) versus those without eczema, with the strongest associations seen for infectious, respiratory, and genitourinary causes.
“Although the absolute risk of death from severe eczema is low, our findings suggest that those with severe or more active forms of the disease do face a higher risk of dying from associated health issues,” a coauthor said in a statement. “We hope that this new information will help inform further research to better understand this pattern and the underlying mechanisms of these associations, and subsequently inform and improve treatment processes for those with severe eczema.”