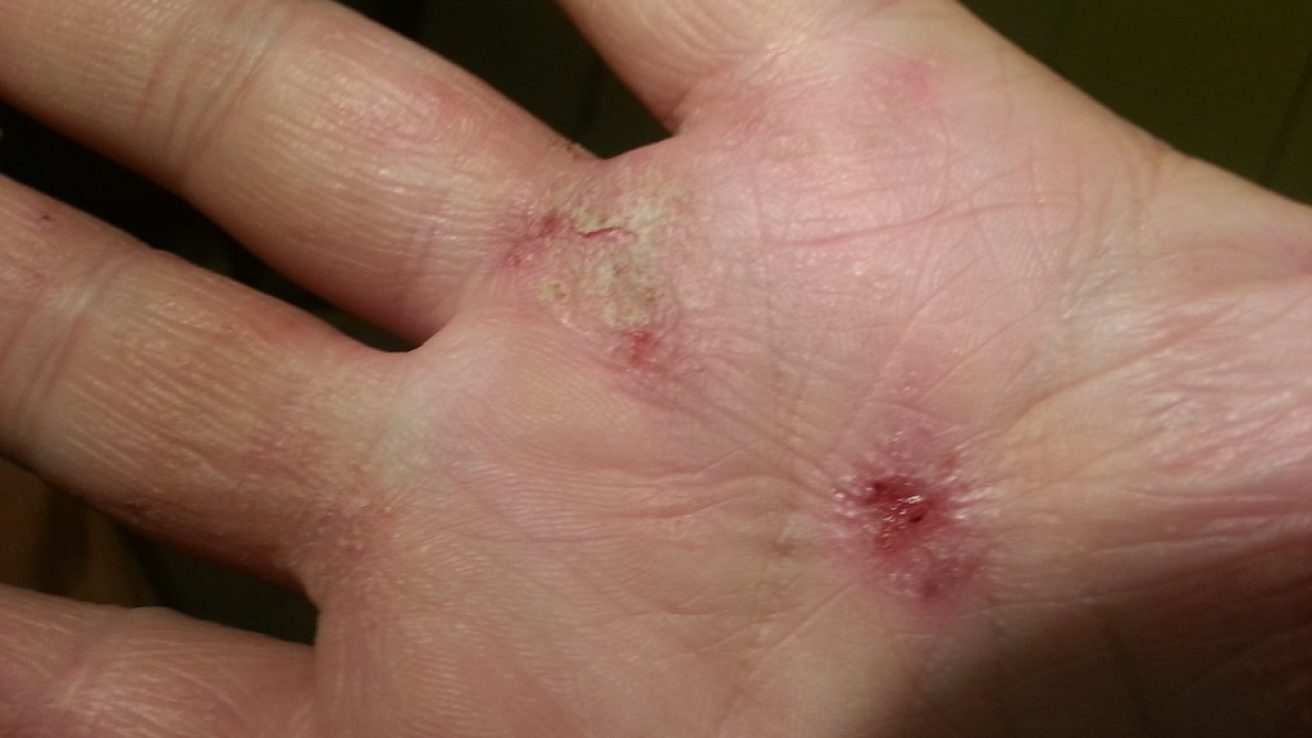
Atopic dermatitis (AD) is a chronic inflammatory skin disease with a usual onset in infancy. While the disease primarily presents during childhood, over 18 million American adults have atopic dermatitis. In the US, African American children have a higher prevalence of AD (20% as compared to 16% among Caucasians) and are also 6-times more likely to have severe AD than white children. [Brunner 2019, Poladian 2019] Conversely, only 8% of African American adults have eczema, compared with 11% of Caucasians, 11% of Hispanics and 9% of Asians. AD is also more prevalent among immigrants with the incidence rapidly rising in developed countries.
AD typically presents with persistent pruritus and has a chronic, relapsing course that includes both flares and remissions. It is characterized by pruritus, xerosis, lichenification and eczematous lesions, with distribution on face, neck and extensors in children, on flexural surfaces in both children and adults but almost always sparing the groin and axillary regions. In African American patients, eczema can result in darker brown, purple, or gray patches, changes in pigmentation and papular eczema on the torso, arms and legs. [Kaufman 2019] Common comorbid conditions in patients with AD include asthma, allergic rhinitis, food allergies and urticaria.
While the pathophysiology of AD is not well defined, there is a definite genetic component to the disease. Theories suggest a combination of immune dysfunction and epithelial barrier disturbance. It is commonly associated with elevated levels of immunoglobulin E (IgE) and other cytokines, including interleukins and interferons. A genetic mutation leading to loss of function in filaggrin, a protein found in skin that is essential in epidermal homeostasis, has been found in up to 50% of European and 27% of Asian patients with AD, but were 6 times less common in African American patients. [Silverberg 2019] Patients with mutations in filaggrin were found to be at increased risk of early-onset, severe, persistent AD with asthma and allergies.
Treatment of AD involves moisturizers, topical steroids, phototherapy, immunomodulators and targeted biologics. Two recently approved agents include crisaborole ointment, a topical phosphodiesterase 4 inhibitor which treats topical lesions, and dupilumab, an injectable biologic therapy that inhibits IL-4 and IL-13 signaling and has been shown to improve disease course. [Silverberg 2019] Treatment must be modified based on patient characteristics, as African American patients require higher doses of cyclosporine A and UV treatment, have an increased incidence of steroid-induced hypopigmentation and are at greater risk of xerosis. [Sanyal 2019]
As AD is a chronic disease and has been associated with a health care burden. This can be especially true of in African American patients, who were found to have higher rate of office visits for AD than white patients. [Sanyal 2019] The chronic nature of AD has been found to put financial strain on patients, due to the high number of office visits and treatment medications needed over the course of the disease. [Koszuru 2019]
AD has been found to affect patient’s quality of life (QOL), with negative impacts on mental health, sleep, physical activity, social functioning, as well as academic and occupational performance. The negative impacts on QOL have been found to be greater in patients of color. [Poladian 2019]
Brunner, Patrick M. et al. Racial differences in atopic dermatitis. Annals of Allergy, Asthma & Immunology. 2019. Volume 122, Issue 5, 449 – 455.
Kaufman B, Alexis A. Eczema in skin of color: What you need to know. https://nationaleczema.org/eczema-in-skin-of-color/.
Koszoru K, Borza J, Gulacsi L, Sarcy M. Quality of Life in Patients With Atopic Dermatitis. Cutis. 2019 September;104(03):174-177.
Poladian K, De Souza B, McMichael AJ. Atopic Dermatitis in Adolescents With Skin of Color In Collaboration With the Skin of Color Society. Cutis. 2019 September;104(03):164-168.
Silverberg JI. Revolutionizing Atopic Dermatitis. Cutis. 2019 September;104(03):142-143
Sanyal RD, et al. Atopic dermatitis in African American patients is TH2/TH22-skewed with TH1/TH17 attenuation. Annals of Allergy, Asthma & Immunology. 2019. Volume 122, Issue 1, 99 – 110.e6