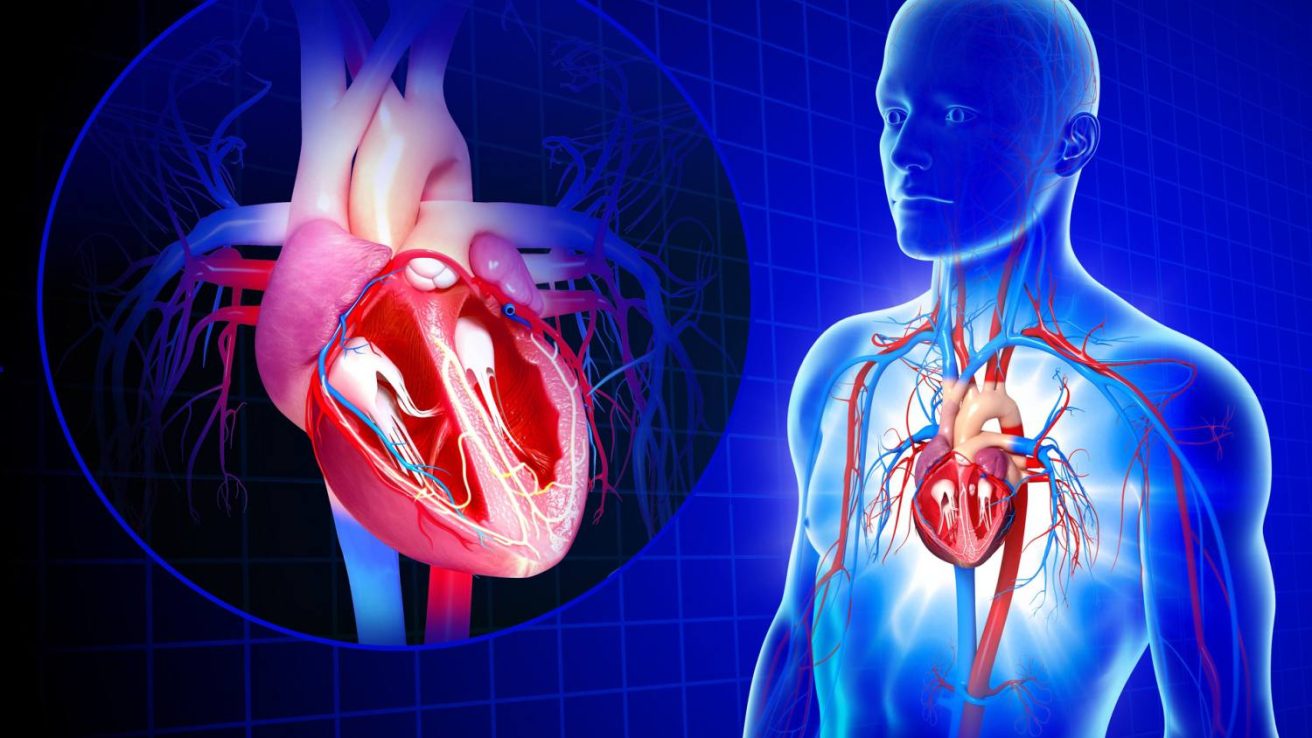
Cardiovascular disease is the leading cause of death of men and women in the United States. Approximately one out of four people or approximately 610,000 people die of heart disease in the United States annually. Similarly, mental health remains a concern worldwide with depression remaining the leading cause of disability worldwide. Depression is highly prevalent among patients with cardiovascular disease with approximately one out of five patients with coronary artery disease or congestive heart failure reporting depression. Stress is also very common among Americans with over two thirds of citizens reporting symptoms of stress on a survey done by American Psychological Association. By treating psychological comorbid conditions, physicians may be able to decrease the risk of progression of cardiovascular disease.
On a cellular level, increased stress levels result in increased nervous system activation along with activation of the immune system resulting in increased inflammatory factors. Additionally there is an increase in cortisol levels and oxidative stress. The cardiovascular system responds by increasing heart rate and blood pressure. If stress levels do not decrease, blood pressure and heart rate may remain persistently elevated resulting in increased risk of cardiovascular disease. Research studies have shown personality traits of hostility, impatience, and urgency are associated with a higher risk of hypertension in African Americans and Caucasians. There has also been shown an increased negative affect among those with hypertension.
It is well known depression can increase the risk of morbidity and mortality in patients with cardiovascular disease. Some studies show a decreased incidence of coronary artery disease among patients with increased positivity and enthusiasm. This is felt to be secondary to better lifestyle habits among patients with positivity. Evidence shows those with increased positivity are more likely to engage in increased physical activity resulting in decreased incidence of coronary artery disease and increased survival rates. Furthermore, researchers feel positivity results in increased alertness, energy, and motivation which promote increased physical activity. Other studies have shown increased smoking cessation among those with increased positive attitude compared to those with a negative mood. Additionally, those with increased positivity may have greater support systems which also promote healthier behaviors.
Cardiac patients with comorbid depression are at increased risk of morbidity and mortality. Patients reporting depression are more likely to have a decreased quality of life and limitations with physical activity. There is an increased risk of future cardiac events among cardiac patients with depression. The association between depression and cardiovascular disease is likely multifactorial secondary to both behavioral and biological mechanisms. Contrary to those with increased positivity, those with depression have decreased physical activity, decreased compliance with medications, and increased smoking. Depression also increases inflammatory response and contributes to autonomic nervous system dysfunction resulting in an increased risk of coronary artery ischemia.
Treatment of cardiovascular disease should include risk factor assessment including psychological health to evaluate presence of depressive disorder and stress levels. It is well known by lowering blood pressure and control of dyslipidemia, there is decreased risk of progression of cardiovascular disease. Similarly, studies suggest by improving the psychological health of cardiac patients, there are decreased morbidity and mortality rates. In order to decrease morbidity and mortality among cardiac patients, medical providers must treat comorbid mental health disorders.
References
Positive affect and health behaviors across five years in patients with coronary artery disease: the heart and soul study by Sin, N. L., Moskowitz, J. T., & Whooley, M. A.
Understanding the correlation between physical activity and clinical depression in women: a review of the literature by Sharpe, D. K., Collins-McNeil, J., Jones, J. W., & Bailey, R. K.
Physical activity, mindfulness medication, or heart rate variability biofeedback for stress reduction: a randomized controlled trial by Van der Zwan, J. E., De Vente, W., Huizink, A. C., Bogels, S. M., & De Bruin, E. I.
State of the art review: depression, stress, anxiety, and cardiovascular disease by Cohen, B. E., Edmondson, D., & Kronish, I. M.
Psychosocial factors are associated with blood pressure progression among African Americans in the Jackson heart study by Ford, C. D., Sims, M., Higginbotham, J. C., Crowther, M. R., Wyatt, S. B., Musani, S. K., …Parton, J. M.
Heart disease facts by Centers for Disease Control and Prevention.