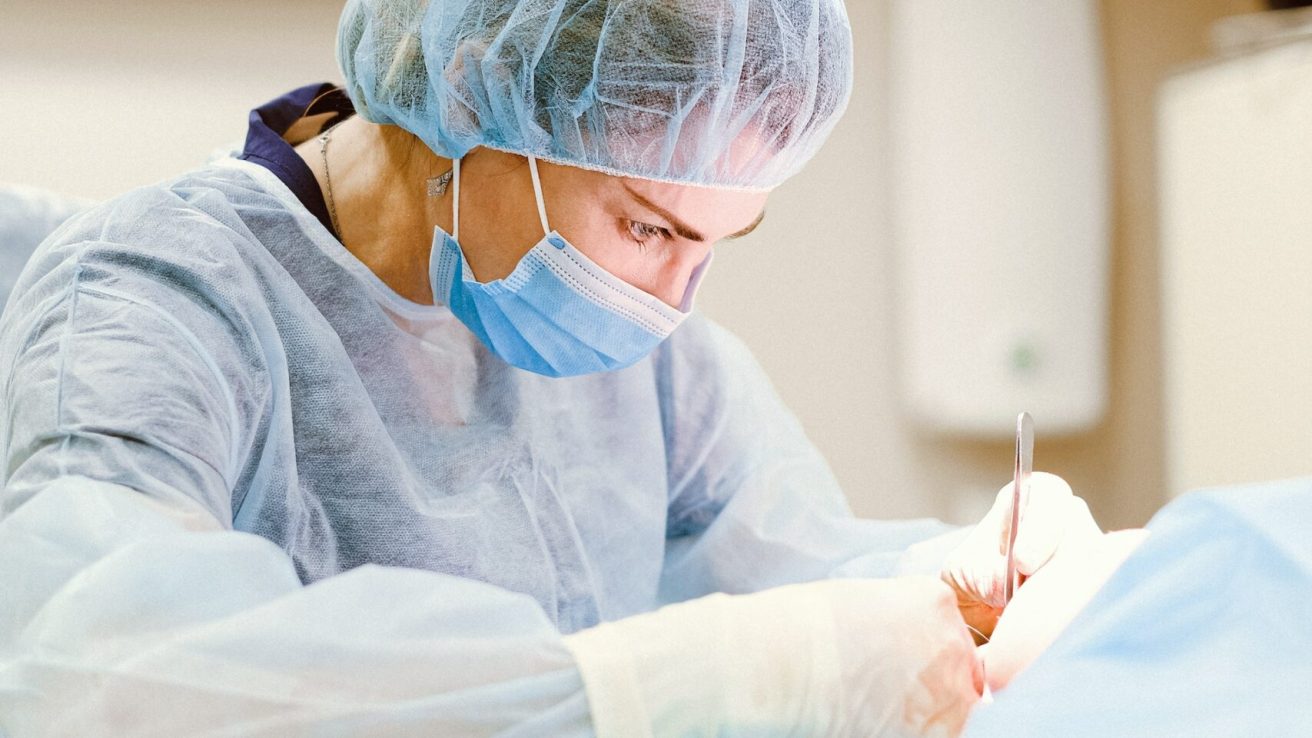
High-flow nasal therapy is a promising therapy for improving oxygenation and patient comfort during transcatheter aortic valve replacement and other medical procedures.
Transcatheter aortic valve replacement (TAVR) is a minimally invasive procedure used to treat aortic stenosis. TAVR patients, who are typically elderly and have multiple health conditions, may experience a common issue of hypoxia.
A study published in the journal Perioperative Medicine demonstrates a comparison between high-flow nasal therapy (HFNT) and standard oxygen therapy (SOT), implying that HFNT does not improve arterial oxygen to a significant extent.
Study Characteristics
This clinical trial compared 72 patients equally divided to receive either HFNT or SOT. The exception of a higher prevalence of prior cardiac surgery in the HFNT group compared to the SOT group (15% vs. 7%, respectively) indicated that twice as many patients had undergone prior cardiac surgery in the HFNT group, and both groups had similar starting characteristics.
Femoral Arterial Line Insertion and Arterial Gas Analysis
Upon insertion of the femoral arterial line, all patients underwent their initial arterial gas analysis. The mean elapsed time from the completion of the pre-surgery checklist to the arterial gas analysis was 51 (SD 16) minutes. The baseline pO2 was found to be lower in the HFNT group when compared to the SOT group, with a median [IQR (range)] of 12.10 (10.05-15.22 (7.2-29.8)) vs. 15.45 (12.17-19.33 (9.2-22.8)) kPa, respectively. Both groups had an inspiratory fraction of oxygen (FiO2) of 0.3, and no significant difference was observed between the two groups in the percentage change in pO2 after 30 minutes (p=0.171).
Comparison of High-Flow Nasal Therapy and Standard Oxygen Therapy After Transcatheter Aortic Valve Replacement
Individuals in the HFNT group stated that they experienced a greater level of comfort and had reduced incidents of oxygen desaturation compared to those who received SOT. However, no significant difference was observed in terms of oxygen requirements and hospital stay duration between the two groups after they underwent TAVR and were in the post-anesthesia care unit.
Both oxygen delivery devices used during the procedure showed no complications, and none of the patients in either group died within the first month after the TAVR procedure.
Outcome Measures
The main parameter used to evaluate the study was the alteration in arterial oxygenation from the initial state to 30 minutes after starting the TAVR procedure. Other factors, such as the frequency of lowered oxygen levels and the level of comfort experienced by the patients, were also considered.
Although the study assessed secondary outcomes, its statistical power was insufficient to draw definitive conclusions, so the results should be considered cautiously. Furthermore, the arterial blood gas measurements could only obtain data at specific time intervals, and for most patients, data were only collected twice. Variations in outcomes may be seen with other high-flow delivery devices or different levels of FiO2 and degree of flow.
Source
Scheuermann, S., Tan, A. L., Govender, P., Mckie, M., Pack, J., Martinez, G., Falter, F., George, S., & Klein, A. A. (2023). High-flow nasal oxygen vs. standard oxygen therapy for patients undergoing transcatheter aortic valve replacement with conscious sedation: a randomised controlled trial. Perioperative Medicine, 12(1). https://doi.org/10.1186/s13741-023-00300-8